E-Mail: sales@microapproachmed.com
Phone: +86-17722685792
- All
- Product Name
- Product Keyword
- Product Model
- Product Summary
- Product Description
- Multi Field Search
E-Mail: sales@microapproachmed.com
Phone: +86-17722685792
Views: 0 Author: Site Editor Publish Time: 2026-02-16 Origin: Site








Urinary tract obstruction is a critical condition that disrupts urine flow and can quickly escalate to severe complications. Left untreated, it may lead to kidney damage or infection.
In this article, we will discuss the most common cause of urinary tract obstructions: urinary stones. You will also learn how Double-J stents are used to restore urine flow and prevent further damage.
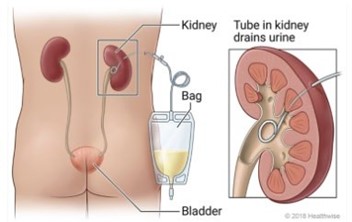
Urine flows from the kidneys through the ureters to the bladder. Any blockage along this path, whether internal (like stones or blood clots) or external (such as tumors or enlarged lymph nodes), can hinder drainage and raise pressure in the kidney. Both types of obstruction can lead to similar symptoms, but their causes and treatments differ. Identifying the cause quickly is key to deciding on the most effective drainage method.
In the short term, obstruction causes pain, nausea, urinary urgency, or reduced urine output. This may happen quickly with a stone or more gradually with a mass compressing the ureter. Obstruction can also lead to infection, which requires urgent decompression. In the long term, persistent pressure can damage the kidneys, especially if not treated. Imaging and lab results help monitor the extent of the damage and guide treatment decisions.
Identifying the cause early is crucial because it helps determine the best treatment path. For example, a stone may need a stent for drainage, while a tumor might require percutaneous drainage. Early identification also allows for timely antibiotic treatment, anesthesia planning, and scheduling definitive procedures, all of which can improve patient outcomes. Ensuring quick access to the right decompression tools, such as stents and guidewires, is essential for minimizing complications.
Urinary stones are the most common cause of urinary tract obstructions because they are prevalent in the general population and because they can move from the kidney into the ureter, where the lumen is narrower and more sensitive to even small changes in diameter. When a stone enters the ureter, it can lodge at anatomical narrow points and create sudden obstruction, which drives a large share of emergency visits and urgent urology consultations, and this clinical visibility reinforces how often stones are the dominant obstruction driver.
Stones also recur in many patients, and recurrent disease increases the probability of future obstruction episodes, which means systems that serve large adult populations often see repeated stone-related blockage cases over time, especially in settings where dehydration, dietary factors, or metabolic conditions are common. This is why a stone-first pathway, supported by rapid imaging and ready-to-use decompression tools, is a practical foundation for obstruction management in many hospitals and surgical centers.
Stone location matters because the ureter is not uniform, and the degree of blockage depends on where the stone is lodged, how tightly it fits, and how much swelling occurs around it. A proximal ureteral stone can cause a rapid rise in renal pelvic pressure and significant hydronephrosis, while a distal stone can trigger urinary frequency, urgency, or bladder discomfort that may initially look like a lower urinary tract problem.
Location also influences how easy it is to place an internal stent, how effective medical expulsive strategies may be, and how urgent decompression becomes when symptoms are severe, because a tight distal obstruction paired with infection can become dangerous quickly even if the patient’s pain is not extreme at presentation. For clinical teams and B2B suppliers, understanding location-driven workflow differences supports better product set planning, since distal ureter cases may require different guidewire handling and access strategies than proximal cases.
Many stone obstructions cause intense flank pain, which is often the symptom that brings patients to care, but not every stone-related obstruction presents in a dramatic way, and that is where risk can increase quietly. Partial obstruction may produce intermittent discomfort, mild urinary symptoms, or vague abdominal pain, and patients may delay evaluation, especially if they have had stones before and assume it will resolve without intervention.
Silent or low-pain obstruction can still damage the kidney if pressure remains elevated, which is why imaging findings and renal function indicators matter as much as symptom intensity, and why clinicians may recommend decompression even when pain seems manageable. From a system standpoint, this also supports the argument for standardized escalation criteria, because relying on pain level alone can lead to under-treatment in patients with significant hydronephrosis or rising creatinine.
Stone risk rises when urine becomes more concentrated or when mineral balance is disrupted, so low fluid intake, high sodium diets, and certain metabolic conditions can increase the chance of stone formation and, by extension, stone-related obstruction episodes. Prior stone history is a practical predictor of recurrence, and patients with repeated stones often benefit from prevention planning, which can reduce future obstruction visits and reduce the need for repeated decompression procedures.
Clinical teams often counsel patients on hydration strategies and diet adjustments, and they may evaluate stone composition when possible, because targeted prevention can be more effective than generic advice. For B2B readers, prevention counseling is still relevant because it affects long-term demand patterns for acute obstruction resources, and it can shift case mix from emergent decompression toward planned outpatient management, which changes what types of urinary diversion device kits are prioritized.
Stone obstruction becomes urgent when there are signs of infection, severe pain with vomiting, very low urine output, obstruction in a solitary kidney, or evidence of declining renal function, because these conditions raise the likelihood of sepsis and permanent kidney injury if drainage is delayed. Obstruction plus fever is especially concerning because bacteria can proliferate behind a blockage, and pressure can push infection into the bloodstream, so clinicians often prioritize decompression over definitive stone removal in the first step when infection risk is high.
In these scenarios, the operational target is quick, reliable drainage using the most appropriate method for the anatomy, which can include internal ureteral stenting or percutaneous nephrostomy, and that is precisely where stocked equipment, trained staff, and standardized decision pathways make a measurable difference in patient safety.
In many clinical summaries and practice environments, stones are repeatedly listed among the leading intrinsic causes of ureteral obstruction, and this aligns with the real-world frequency of stone-related emergency presentations, imaging-confirmed ureteral stones, and urgent decompression cases. Even though other causes like tumors and strictures can be severe, they occur less frequently in broad adult populations than stones, and their progression is often slower, which means they account for a smaller share of sudden, high-acuity obstruction events.
Benign prostatic enlargement is common in older men and can obstruct urine flow at the bladder neck, leading to bladder retention and possible dilation of the upper urinary tract. While this condition is common, it does not surpass stones as the leading cause of urinary tract obstructions in broader populations. Symptoms usually include weak urine flow, incomplete bladder emptying, and frequent urination, rather than the sudden flank pain typical of stone obstructions.
Tumors can either grow within the urinary tract or compress the ureter from the outside, obstructing urine flow. These cases are more complex because the obstruction’s location must be carefully considered, and drainage methods like stenting or percutaneous drainage may be necessary. Symptoms develop gradually and may include weight loss, hematuria, or urinary changes, with imaging used to assess the extent of obstruction and invasion.
Congenital conditions, like ureterocele or ureteral junction narrowing, can cause obstructions from birth or early childhood and often require surgical correction. In adults, acquired causes, especially stones, dominate as the leading trigger for acute ureteral obstruction. The treatment pathway for congenital cases often involves pediatric care, while adults typically undergo more immediate interventions for stone-related blockages.
While other causes like prostate enlargement, tumors, and congenital abnormalities are clinically significant, they occur in narrower patient groups. Stones, however, affect a wide range of people and can develop suddenly in otherwise healthy individuals. This broader impact is why stones remain the most common cause of urinary tract obstructions, even though other causes may present more complex cases.
Cause category | Typical onset pattern | Common first-step response | Why it matters for equipment planning |
Urinary stones | Sudden, high-acuity in many cases | Rapid imaging and decompression if needed | High-volume pathway needs stents, guidewires, and flexible kits |
Prostate enlargement | Gradual, retention-focused | Bladder drainage and medication evaluation | Requires catheter readiness and lower-tract workflow support |
Tumors/compression | Often progressive, high complexity | Drainage plus diagnostic workup | Needs both stent and nephrostomy options, plus imaging support |
Congenital narrowing | Early-life detection or incidental findings | Stabilize, then definitive correction planning | Pediatric sizing and specialized protocols may apply |
A urinary diversion device is used to restore or bypass urine flow when the normal pathway is blocked, and it serves as a stabilizing step that reduces renal pelvic pressure, improves drainage, and lowers the risk of ongoing renal injury while clinicians plan definitive treatment. In many obstruction scenarios, diversion is not the final cure, but it is the critical bridge that prevents deterioration, especially when infection is present or when definitive stone removal cannot occur immediately due to patient condition, operating room availability, or required imaging and planning.

Ureteral stents create an internal drainage path from kidney to bladder, nephrostomy tubes drain urine externally from the kidney, and bladder catheters relieve lower-tract retention, so each option fits a different anatomical and clinical situation. In stone-related ureteral obstruction, ureteral stents are commonly used when retrograde access is feasible, while nephrostomy may be preferred when access is difficult or when a rapid external drain is judged to be the most reliable option for decompression.
Most diversion devices used for stones are temporary because the ultimate goal is stone passage, extraction, or fragmentation, and diversion simply protects the kidney and stabilizes symptoms while the definitive plan is executed. Long-term diversion is more common in malignancy-related obstruction or chronic strictures, where repeated stent exchanges or ongoing external drainage may be required to preserve renal function in the context of a persistent obstructing condition.
Early diversion reduces back pressure and urinary stasis, which can lower infection risk and protect kidney function, and it also creates time for safer, better-planned definitive treatment rather than forcing rushed procedures under unstable clinical conditions. From a B2B perspective, early diversion success often depends on having a complete “placement ecosystem,” including the right stent types, compatible guidewires, pushers, and packaging that supports sterile and efficient workflow, rather than having only the primary device without critical accessories.
Imaging is essential for diagnosing urinary tract obstructions. It helps confirm hydronephrosis, locate the blockage, and differentiate stones from other causes like tumors or strictures. Ultrasound is commonly used to detect swelling and provide quick bedside information. CT imaging offers more precise details and clarifies anatomy when planning procedures.
Imaging also helps determine if retrograde access is possible or if percutaneous drainage is needed for rapid decompression. Ensuring access to imaging tools is critical for effective obstruction management.
Lab tests, such as creatinine levels and urinalysis, help assess kidney function and infection. Rising creatinine suggests kidney stress, while urinalysis can reveal hematuria or infection markers. When obstruction and infection occur together, timely decompression and antibiotic treatment are prioritized. Lab results also track recovery after drainage, especially in patients with severe symptoms.
Stones typically cause sudden pain and are visible in imaging. Tumors and strictures tend to cause gradual obstruction and progressive hydronephrosis. A patient’s medical history—such as previous surgeries or cancer treatments—can indicate whether strictures or tumors are more likely, which helps guide the drainage method.
The cause and location of the obstruction guide the choice of urinary diversion device. For ureteral stones, Double-J stents are often used for internal drainage, as they maintain patient mobility. In cases where stenting is not possible, percutaneous drainage may be used. Bladder catheter drainage is typically reserved for outlet obstructions, not ureteral blockages.
Urinary tract obstructions, especially those caused by urinary stones, can severely impact kidney function if not addressed promptly. Early diagnosis and treatment are crucial to preventing long-term damage.
A Double-J stent plays a key role in restoring urine flow and protecting the kidneys. Shenzhen MicroApproach Medical Technology Co., Ltd. offers high-quality Double-J stents and other urinary diversion devices that provide reliable drainage and support for patients. Their products are designed for smooth insertion and minimal complications, helping healthcare providers manage obstructions effectively.
By choosing Shenzhen MicroApproach Medical Technology Co., Ltd., clinicians can ensure timely and efficient treatment for urinary tract obstructions, improving patient outcomes and enhancing care quality.
A: The most common cause of urinary tract obstructions is urinary stones, which can move from the kidneys to the ureters, causing a blockage. This leads to increased pressure in the kidney, potentially resulting in pain or kidney damage if untreated.
A: Double-J stents are used to restore urine flow in cases of ureteral obstruction caused by stones. They are inserted into the ureter to bypass the blockage, allowing urine to drain from the kidney to the bladder and preventing kidney damage.
A: Double-J stents are commonly used because they offer a reliable method for maintaining drainage in the ureter. Their pigtail design helps prevent migration, and their radiopaque material allows easy imaging for placement confirmation.
A: Double-J stents are typically used for temporary management of urinary tract obstructions. They help relieve pressure while the underlying issue is treated. Long-term stenting may be required in certain chronic cases, such as recurrent obstructions or malignancy.
14 Jinhui Road, Pingshan District, Shenzhen,518122, P.R.China
+86-755-89459010
+86-18320758765 Ares
+86-15013496274 Daisy
+86-15813727825 Gloria